
A volunteer is sitting in an office in Binghamton, New York. She’s wearing a sundress. So there’s no need to roll up a sleeve. A researcher walks in and gives her a shot. “Well, that was painless,” the volunteer says, cheerfully.
That was July 27, the day the first potential coronavirus vaccine reached late-stage testing in the United States. It was made by Moderna and the National Institutes of Health. Human trials
trial
 AMPHOTORA—GETTY IMAGES
a test of the quality, value, or usefulness of something
(noun)
A clinical trial showed that the drug was safe and helpful.
began in March. Tens of thousands of volunteers would sign up. Now, two more companies have reached late-stage vaccine testing in the U.S.
AMPHOTORA—GETTY IMAGES
a test of the quality, value, or usefulness of something
(noun)
A clinical trial showed that the drug was safe and helpful.
began in March. Tens of thousands of volunteers would sign up. Now, two more companies have reached late-stage vaccine testing in the U.S.

VACCINE TESTING Some vaccine trials are taking place at the Research Centers of America, in Hollywood, Florida.
CHANDAN KHANNA—AFP/GETTY IMAGESA vaccine would protect people from COVID-19. With enough people inoculated
inoculate
 FATCAMERA—GETTY IMAGES
to protect from disease
(verb)
We took our dog to the veterinarian so she could be inoculated against rabies.
, it would save lives. It would help end the pandemic. That’s why there’s a rush to develop it.
FATCAMERA—GETTY IMAGES
to protect from disease
(verb)
We took our dog to the veterinarian so she could be inoculated against rabies.
, it would save lives. It would help end the pandemic. That’s why there’s a rush to develop it.
Need for Speed
A vaccine builds our immunity
immunity
 CHOJA—GETTY IMAGES
freedom from sickness or harm
(noun)
Because I had chickenpox last year, I now have immunity from it.
to a virus. “It teaches the body to recognize the virus,” Dr. Rick Malley told TIME for Kids. Malley works at Boston Children’s Hospital. That’s in Massachusetts. “The next time the body sees the bug,” he says, “it fights it off without ever getting sick.”
CHOJA—GETTY IMAGES
freedom from sickness or harm
(noun)
Because I had chickenpox last year, I now have immunity from it.
to a virus. “It teaches the body to recognize the virus,” Dr. Rick Malley told TIME for Kids. Malley works at Boston Children’s Hospital. That’s in Massachusetts. “The next time the body sees the bug,” he says, “it fights it off without ever getting sick.”
It can take 10 years to develop a vaccine (see “Road to Success”). Scientists have to do research. They have to produce a vaccine they can test. It must pass three phases of human trials. Then it can be approved, manufactured, and distributed.
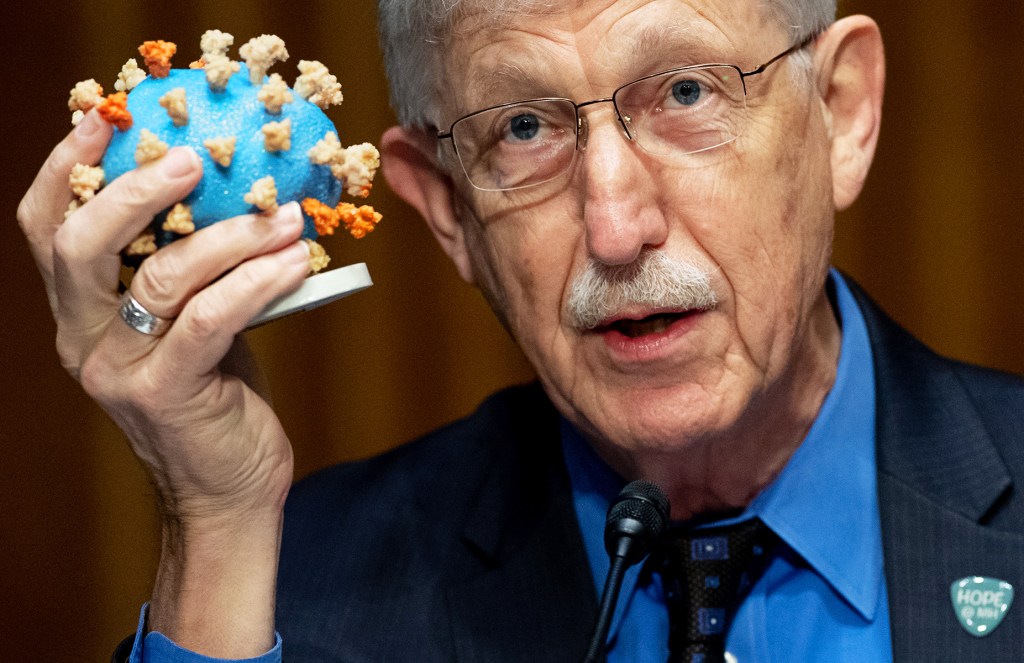
FIGHTING THE VIRUS Dr. Francis Collins, of the National Institutes of Health, speaks about Operation Warp Speed in Washington, D.C., on July 2.
SAUL LOEB—AFP/BLOOMBERG/GETTY IMAGESOperation Warp Speed has made this process faster. The U.S. government launched the program in May. It gives billions of dollars to companies so they can quickly make coronavirus vaccines.
Some companies have used money from Operation Warp Speed to manufacture doses of a vaccine before the final phase of testing is complete. If it’s safe and effective, the vaccine can then be distributed right away.
Down the Line
It’s uncertain when a vaccine will be ready in the U.S. Robert Redfield is director of the Centers for Disease Control and Prevention. On September 2, he spoke to Yahoo Finance. Redfield said “one or more vaccines” could be ready by the end of the year.
Moncef Slaoui is a scientist. He’s one of the leaders of Operation Warp Speed. On August 31, he spoke to National Public Radio. Slaoui said that “we may have enough vaccine by the end of the year [for] between 20 [million] and 25 million people.”
That means many people will have to wait. The first doses will likely go to health-care workers and elderly people. “We have to figure out how to make sure they’re distributed in a fair and equitable
equitable
 FLORESCO PRODUCTIONS/GETTY IMAGES
fair and equal
(adjective)
Teachers should have an equitable system for giving students detention.
way,” Redfield says.
FLORESCO PRODUCTIONS/GETTY IMAGES
fair and equal
(adjective)
Teachers should have an equitable system for giving students detention.
way,” Redfield says.
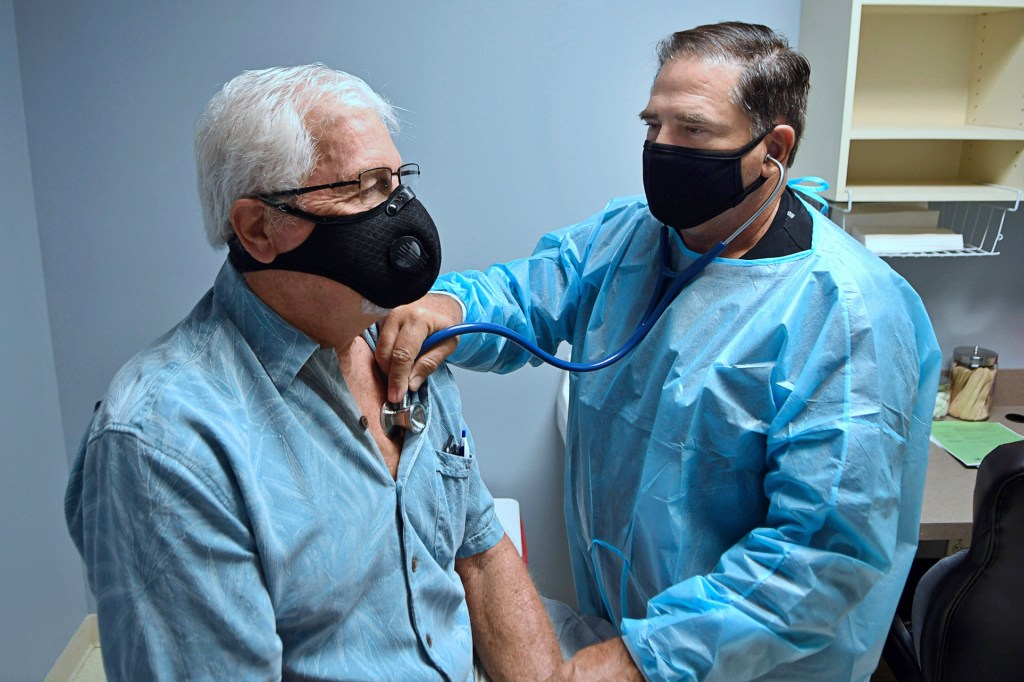
PUT TO THE TEST On August 4, a volunteer is examined before participating in a coronavirus vaccine trial in DeLand, Florida.
PAUL HENNESSY—NURPHOTO/GETTY IMAGESOther countries are working on vaccines too. Australia, China, India, Italy, Japan, Russia, Singapore, and South Korea are in the human-trials stages.
As the U.S. races toward a vaccine, safety is a top concern. On September 8, the leaders of nine companies working on vaccines in the U.S. issued a statement: They won’t release a vaccine before they’re sure it’s safe. They promise to make “the safety and well-being of vaccinated individuals our top priority.”
Road to Success
Making a new vaccine takes a lot of work. Here are the five steps.
Before trials: Scientists conduct research. They run early tests on cells and animals.
Phase 1: The vaccine is tested on a small group of human volunteers to make sure it’s safe.
Phase 2: The vaccine is tested on a slightly larger group of volunteers. This is to check for safety again.
Phase 3: The vaccine is tested on thousands of volunteers. Researchers find out if the vaccine is effective.
After trials: A vaccine may now be approved by the government. It can then be manufactured and distributed to the public.












